Adderall addiction can develop even in people who start with a valid prescription, and recognizing it early makes a real difference in outcomes.
About 4.3 million people in the United States had a stimulant use disorder in a recent year, and prescription stimulant misuse has become a growing public health concern, especially among young adults.
This article walks through the clearest signs, physical and psychological symptoms, long-term effects, withdrawal, and the treatments with the strongest evidence behind them.
Adderall Addiction Signs You Should Know
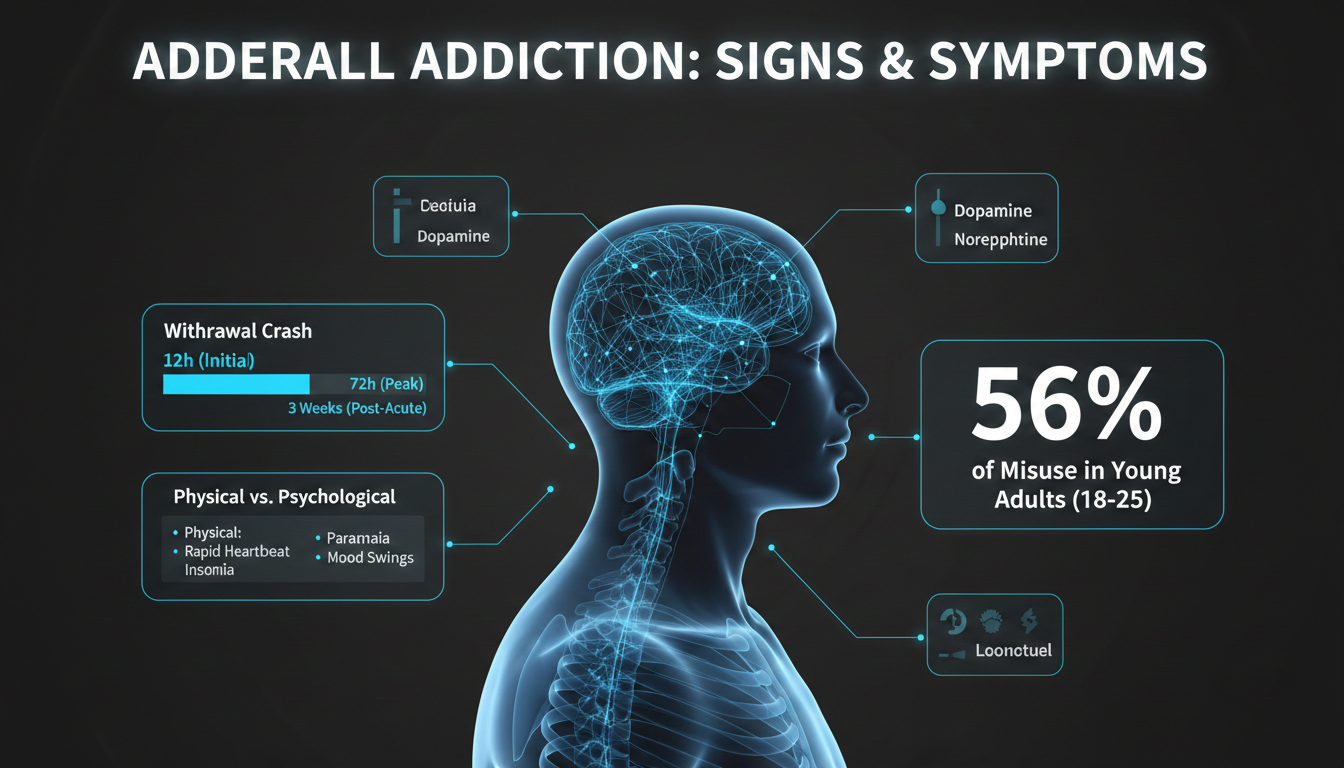
Adderall is a Schedule II prescription stimulant containing mixed amphetamine salts. It is FDA-approved for ADHD and narcolepsy, and it works by increasing dopamine and norepinephrine activity in the brain. That same mechanism is what makes it effective and what makes it risky when misused.
The clearest marker that use has become a problem is not “taking Adderall” but losing control over it. Stimulant use disorder is diagnosed when a person meets at least two of eleven clinical criteria within a twelve-month period, including inability to reduce use, cravings, continuing use despite relationship problems, and needing increasing amounts to get the same effect.
A valid prescription does not remove that risk. Someone can develop Adderall addiction even while using it as prescribed, particularly when doses escalate, use spreads beyond its intended purpose, or the person begins to feel unable to function without it.
Behavioral Warning Signs
The behavioral signs of Adderall addiction tend to appear before the physical ones become obvious:
- Taking larger amounts or using more often than intended
- Repeated failed attempts to cut back or stop
- Spending a lot of time getting, using, or recovering from Adderall
- Running out of a prescription early
- Doctor shopping or visiting multiple prescribers to get extra supply
- Using someone else’s prescription
- Hiding use or lying about how much is being taken
- Continuing to use despite knowing it is causing physical or psychological harm
- Giving up activities, hobbies, or relationships that once mattered
Doctor shopping deserves special attention because it appears in both clinical and treatment-oriented sources as a recognized misuse indicator.
StatPearls notes that pharmacists should monitor prescribing patterns and alert clinicians to potential doctor shopping as a sign of medication misuse.
Snorting or injecting Adderall is another serious behavioral marker. It signals a higher-intensity pattern of use driven by the pursuit of rapid onset and euphoria, and it substantially raises the risk of overdose and addiction.
Who is Most at Risk?
Young adults and college students face the highest risk of nonmedical Adderall use. In 2018, over 4.6 million people misused prescription amphetamine products in the past year, and young adults aged 18 to 25 made up 56 percent of those taking them for nonmedical reasons.
Full-time college students are twice as likely to use Adderall non-medically as same-age peers who are not in school.
Other elevated-risk groups include people under academic or professional pressure, those with a history of substance misuse, and people with co-occurring mood disorders such as depression or anxiety.
Adderall Addiction Symptoms: Physical and Psychological
Adderall addiction symptoms span the body and the mind. Physical symptoms alone do not confirm addiction, but when they appear alongside loss of control and continued use despite harm, the picture becomes much clearer.
Physical Symptoms
- Insomnia or severely disrupted sleep
- Significant appetite suppression and weight loss
- Rapid heartbeat or irregular heart rhythm
- High blood pressure
- Chest pain
- Headaches, nausea, or stomach upset
- Tremor or muscle tension
- Dry mouth
- Dilated pupils
Cardiovascular symptoms deserve particular emphasis. Yale Medicine notes that heavy stimulant use can cause irregular heartbeat, heart failure, seizures, and death.
StatPearls warns that sudden death and severe cardiovascular events are major concerns with amphetamine use in patients with structural cardiac abnormalities. Chest pain, marked rapid heartbeat, or severe high blood pressure should never be dismissed as ordinary stimulant side effects.
Psychological and Adderall Addiction Symptoms
- Anxiety and irritability
- Mood swings, often cycling between euphoria during use and deep dysphoria when it wears off
- Depression or emotional flatness
- Difficulty concentrating or slowed thinking as tolerance builds
- Paranoia
- In severe cases, hallucinations or psychosis
The mood cycling pattern is clinically important. Someone who felt sharp and energized while using Adderall may feel profoundly low, foggy, and unmotivated between doses. That contrast reinforces continued use and makes stopping feel impossible.
Paranoia, hallucinations, and psychosis are not late but routine signs. They are severe warning signs that need urgent psychiatric assessment.
Adderall Addiction Side Effects on Daily Life
Beyond the body and mind, Adderall addiction side effects ripple into every area of functioning:
- Declining performance at work or school
- Missed deadlines, absences, or neglected responsibilities
- Social withdrawal and shrinking relationships
- Financial problems from spending money on the drug
- Neglect of personal hygiene and basic self-care
- Relationship conflict and erosion of trust
When functioning declines in these ways, the practical costs of use are already established. Waiting for a more dramatic crisis before seeking help is not supported by the evidence.
Adderall Addiction Withdrawal Symptoms
When someone who has been using Adderall heavily stops or sharply reduces use, the brain, which has adapted to the drug’s presence, no longer has the same external drive.
The result is a withdrawal syndrome that is less about dramatic physical collapse and more about a profound neuropsychological crash.
The Cochrane review on amphetamine withdrawal describes the initial crash as involving severe dysphoria, irritability, anxiety, hypersomnia, marked fatigue, intense craving, and in some cases paranoia. Adderall addiction withdrawal symptoms typically follow a rough progression:
- Within 12 to 24 hours: sleepiness and irritability begin as catecholamine levels drop
- First week: profound fatigue, sleeping much more than usual, increased appetite, depressed mood, anxiety, poor sleep quality, and strong cravings
- One to three weeks: ongoing fatigue, concentration problems, insomnia, anxiety, and continued craving
- Weeks to months: post-acute symptoms including depression, anxiety, insomnia, paranoia, and low motivation that can persist long after the acute phase ends
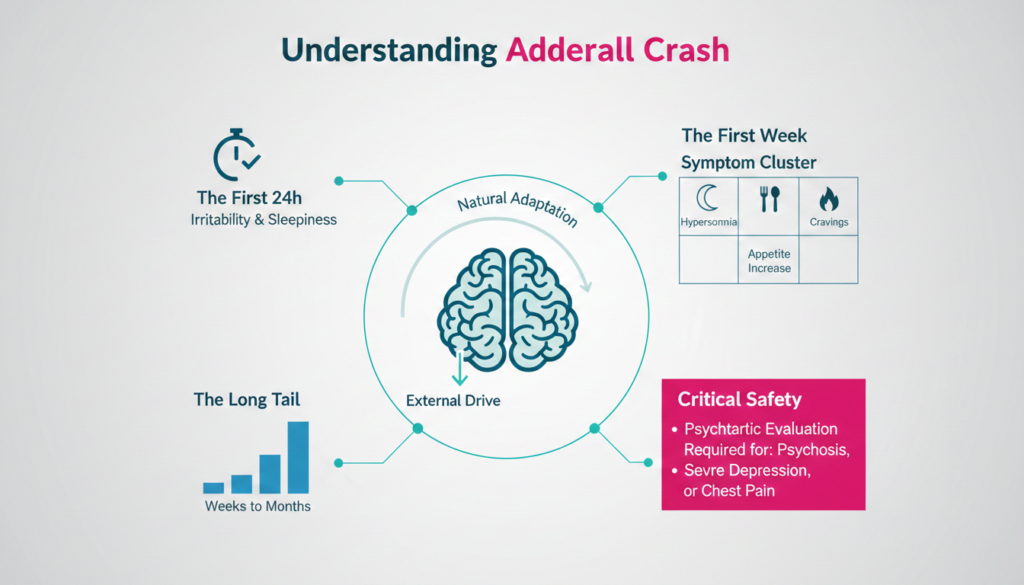
The 2024 ASAM/AAAP clinical practice guideline on stimulant use disorder confirms that post-acute withdrawal symptoms can last for weeks to months and raise the risk of relapse and psychiatric decompensation if left unaddressed.
Suicidal thoughts and attempts have been reported during amphetamine withdrawal. Anyone experiencing severe depression, thoughts of self-harm, psychosis, or chest pain during withdrawal needs immediate medical or psychiatric evaluation.
Adderall Addiction Treatment: What the Evidence Shows?
The most important thing to understand about adderall addiction treatment is that detox alone is not enough. Stopping the drug is the beginning, not the solution.
The strongest evidence points to structured behavioral treatment as the foundation of recovery, not medication.
Contingency Management: The Current Standard of Care
The ASAM/AAAP guideline calls contingency management the current standard of care for stimulant use disorder. A systematic review of reviews on stimulant use disorder treatments found sufficient evidence to support contingency management, while evidence for most pharmacologic approaches was insufficient.
Contingency management uses positive reinforcement, such as vouchers, prizes, or gift cards, for desired behaviors like stimulant-negative urine tests or consistent treatment attendance.
In a randomized controlled trial in community mental health settings, participants in contingency management were 2.4 times more likely to submit stimulant-free urine samples during treatment and had 40 percent more substance-free samples after treatment, along with fewer psychiatric hospitalizations.
This approach works especially well for stimulant addiction because it directly competes with the immediate reinforcement that the drug provides.
Cognitive Behavioral Therapy
CBT helps people identify triggers, challenge distorted thinking, build coping skills, and develop relapse prevention strategies.
For Adderall specifically, it can address beliefs like “I cannot study or work without it,” manage high-pressure situations that drove use, and rebuild daily routines after dependence.
CBT is most effective when combined with contingency management. CM helps generate early abstinence and engagement; CBT builds the skills that sustain recovery once external rewards taper.
Other Behavioral Approaches
The Community Reinforcement Approach aims to make sober living more rewarding than drug use by addressing social, vocational, and environmental factors.
The Matrix Model combines structured counseling, CBT, family education, and relapse prevention, and evidence suggests it improves treatment retention and during-treatment abstinence.
Motivational interviewing and family involvement are useful adjuncts, particularly for younger adults where family dynamics and academic pressure intersect with stimulant misuse.
Adderall Addiction Treatment and Medication
There is currently no FDA-approved medication specifically for stimulant use disorder. The ASAM/AAAP guideline is clear on this point, and the systematic review of reviews found insufficient evidence to support most pharmacologic options as primary treatment.
Medications can still play a supportive role. Clinicians may use them to manage specific withdrawal symptoms such as insomnia, depression, anxiety, agitation, or psychosis.
In carefully selected cases with co-occurring ADHD, a specialist may consider prescribed psychostimulants under close monitoring, including pill counts, drug testing, and more frequent clinical contact. But medication is not the main answer for most people seeking Adderall addiction recovery.
Levels of Care
Treatment intensity should match clinical need. Options include:
- Inpatient or residential treatment for 24-hour monitoring and structured support
- Partial hospitalization programs for intensive daily treatment without overnight stays
- Intensive outpatient programs for structured therapy while living at home
- Standard outpatient programs for ongoing therapy and monitoring
- Continuing care and aftercare planning to support long-term recovery
People with suicidal thoughts, psychosis, severe functional collapse, or repeated relapse may need higher levels of care.
Stable individuals with strong support systems may recover effectively in outpatient settings if evidence-based therapies are available.

Adderall Addiction Recovery: What to Expect?
Adderall addiction recovery is not a straight line. The post-acute phase, which can last weeks to months, often brings depression, insomnia, anxiety, cognitive slowing, low motivation, and intermittent cravings. Many people feel that sobriety itself feels empty or mentally impaired during this period.
That is why SAMHSA’s SBIRT framework emphasizes early identification and intervention before severe consequences develop. Waiting for catastrophic outcomes before seeking help is neither evidence-based nor necessary.
Recovery plans that only address the first week of withdrawal are inadequate. The strongest treatment models assume that the person may not feel normal quickly and plan for that reality with continuing care, psychiatric monitoring, and structured behavioral support.
The most defensible conclusion from the evidence is this: Adderall use has become a problem when the drug controls the person more than the person controls the drug.
And the most effective path forward is not willpower or detox alone, but a structured, multi-phase care plan centered on contingency management, CBT, and close attention to co-occurring mental health needs.
If you or someone you care about is showing signs of Adderall addiction, reaching out to a treatment team is the most important next step.
Thoroughbred Wellness and Recovery offers a full continuum of care, from medical detox through outpatient programs, with dual diagnosis support and evidence-based therapies. You can learn more or start the conversation with our team today!









