
Stopping alcohol after heavy use can trigger withdrawal symptoms that range from uncomfortable to life-threatening. Many people wonder whether they can safely detox at home, but the answer depends on your individual risk factors, medical history, and support system.
According to the American Society of Addiction Medicine, some carefully selected patients with mild symptoms and no history of complications can undergo ambulatory withdrawal management, but home detox becomes unsafe when there is elevated risk for severe withdrawal, significant medical or psychiatric illness, or inadequate monitoring.
This article explains who can safely detox at home, which warning signs indicate danger, and when professional medical care is essential.
Understanding Alcohol Withdrawal and Why It’s Dangerous?
Alcohol withdrawal is not simply discomfort after quitting drinking. It is a neurophysiologic rebound syndrome that occurs when your brain, adapted to chronic alcohol exposure, suddenly loses that depressant effect.
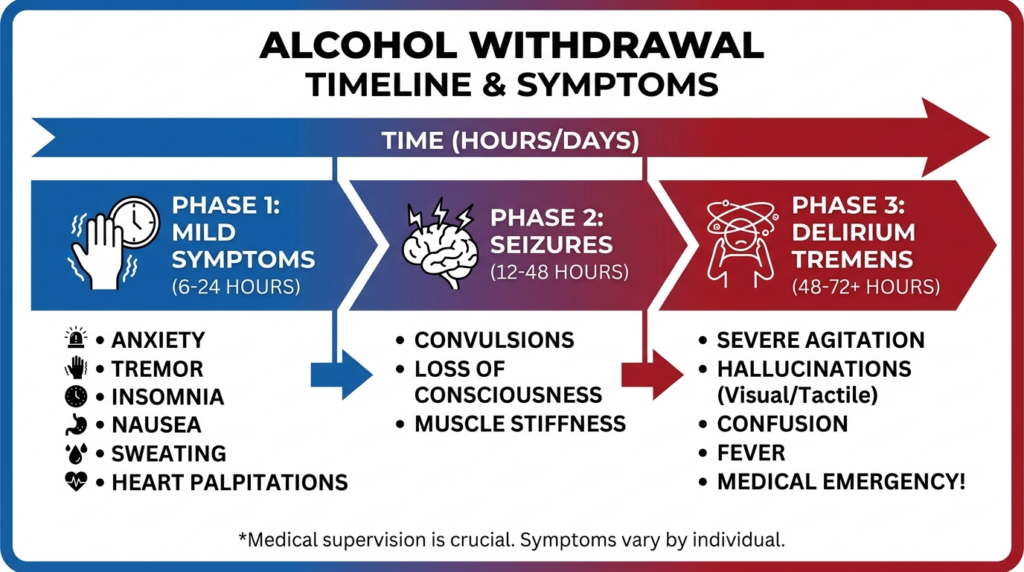
The result is a hyperexcitable state that can produce tremor, sweating, anxiety, rapid heart rate, high blood pressure, hallucinations, seizures, and delirium tremens.
The National Institute for Health and Care Excellence emphasizes that withdrawal severity exists on a spectrum. Early symptoms may seem manageable, but they can escalate rapidly.
Seizures typically occur within 6 to 48 hours after the last drink, with peak risk around 24 hours. Delirium tremens, the most severe form of withdrawal, usually emerges 48 to 72 hours after cessation and carries a mortality risk of 1% to 5% even with treatment.
This delayed progression is one of the biggest dangers of home detox. You may feel only mildly anxious and shaky on the first day, assume the worst is over, and then experience a seizure or severe confusion the next day. That timeline makes unsupervised home detox especially risky.
When Home Detox May Be Appropriate?
Home-based alcohol withdrawal management is not inherently impossible, but it requires careful risk assessment and structured support.
The evidence shows that ambulatory detox can be reasonable for a narrow group of people who meet all of the following criteria:
- Mild to moderate withdrawal symptoms with no confusion, hallucinations, or seizure activity
- No history of withdrawal seizures or delirium tremens
- No significant medical problems such as liver disease, heart disease, infection, or head injury
- No major psychiatric instability, suicidality, or cognitive impairment
- A stable, alcohol-free home environment
- A reliable support person who can monitor symptoms daily
- Ability to attend daily or every-other-day follow-up with a clinician
- Rapid access to emergency care if symptoms worsen
According to ASAM’s clinical practice guideline, even when these conditions are met, ambulatory management should include daily check-ins for up to five days, validated symptom monitoring, thiamine supplementation, medication when indicated, and clear criteria for transfer to a higher level of care.
This is fundamentally different from attempting to “tough it out” alone at home. Structured ambulatory withdrawal is a medical program with professional oversight, not a do-it-yourself strategy.
The Biggest Risks of Detoxing From Alcohol at Home
1. Seizures
Withdrawal seizures are among the most feared complications because they can occur with little warning and may lead to head injury, aspiration, recurrent seizures, or progression to delirium. Harvard Health notes that seizures can happen 6 to 48 hours after the last drink, often clustering over several hours.
At home, there is no immediate medical response, no IV access for medication, and no monitoring for postictal confusion or evolving delirium. A person may fall and strike their head, or family members may misinterpret the seizure as fainting or intoxication.
2. Delirium Tremens and Altered Mental Status
Delirium tremens involves severe confusion, disorientation, hallucinations, and autonomic instability. It is a true medical emergency that may require ICU-level care, IV benzodiazepines, continuous monitoring, and airway management. Home settings are poorly equipped to handle this level of acuity.
Because DTs usually occur later than early withdrawal symptoms, patients and families may falsely conclude the situation is improving. Also, altered mental status itself reduces the reliability of self-reported symptoms and makes it difficult to follow treatment instructions.
3. Misjudging Risk Based on Current Symptoms
One of the most dangerous mistakes is assuming that mild current symptoms mean low risk. The Prediction of Alcohol Withdrawal Severity Scale was developed specifically because common tools like CIWA-Ar quantify present severity but do not identify who is at risk of deterioration before symptoms escalate.
A person may have only mild anxiety and tremor at hour 10 but still be at high risk for seizures or delirium if they have a history of prior complicated withdrawal, multiple prior detoxifications, heavy daily intake, liver disease, older age, or comorbid illness. Risk prediction matters as much as current symptom measurement.
4. Prior Complicated Withdrawal and Kindling
Repeated withdrawals increase future severity risk through a phenomenon called kindling, in which prior withdrawal episodes sensitize the nervous system. The American Family Physician notes that prior withdrawal seizures and delirium tremens are among the strongest predictors of future complications.
This means your withdrawal history is not just background information. It is one of the most important risk factors. A history of prior withdrawal seizures or DTs should be treated as a near-disqualifier for unsupervised home detox.
5. Medical Comorbidities and Unstable Chronic Disease
Alcohol-dependent patients frequently have concurrent medical issues such as liver disease, pancreatitis, gastrointestinal bleeding, cardiomyopathy, electrolyte abnormalities, nutritional deficiencies, infections, or trauma. Withdrawal can mimic or mask other dangerous conditions, especially if the patient is confused, intoxicated, or injured.
A 2025 prospective study found that previous delirium tremens and increased liver stiffness were significant risk factors for severe alcohol withdrawal. Home detox is dangerous in this group because the patient may not only worsen from withdrawal but also decompensate from the underlying illness.
6. Psychiatric Illness, Suicidality, and Cognitive Impairment
ASAM states that active suicide risk generally necessitates treatment in a setting equipped to manage that risk, often inpatient psychiatric care with withdrawal management capability. It also identifies moderate or severe psychiatric symptoms and cognitive impairment as factors arguing against low-acuity ambulatory care.
Psychiatric instability raises home-detox risk through unreliable symptom reporting, poor medication adherence, impulsivity or self-harm risk, confusion between withdrawal and psychiatric symptoms, and limited ability to seek help if deterioration occurs.
7. Lack of Reliable Support Network
A lack of reliable support is repeatedly cited as a relative indication for inpatient detoxification. Home monitoring is inadequate when there is no one available to notice worsening tremor, confusion, seizures, resumed drinking while taking benzodiazepines, or failure to take thiamine and medications properly.
This is not a minor social issue. It directly affects monitoring frequency, medication supervision, recognition of hallucinations or confusion, emergency response if seizure occurs, and prevention of relapse during the withdrawal window.
8. Inadequate Hydration, Nutrition, and Thiamine Replacement
Supportive care is integral to safety. ASAM recommends thiamine for patients in withdrawal, especially IV or IM in high-risk or hospitalized patients, to prevent Wernicke encephalopathy. Typical ambulatory oral thiamine is 100 mg daily for 3 to 5 days.
At home, patients may be vomiting, sweating, not eating, and trying to “sleep it off.” That combination can worsen dehydration, hypoglycemia, and electrolyte disturbance, which independently increase seizure and arrhythmia risk.
9. Unsafe Self-Medication
Unsupervised sedative use can cause oversedation, misuse, and masking of worsening withdrawal. Guidelines recommend structured benzodiazepine regimens and supervision. Patients sometimes try to self-manage with benzodiazepines obtained from prior prescriptions, friends, or illicit sources, creating risks of respiratory compromise and poorly controlled withdrawal.
10. Failure to Transition to Long-Term Treatment
ASAM strongly emphasizes that withdrawal management should initiate and engage patients in ongoing alcohol use disorder treatment rather than stand alone. Repeated unsupported detox attempts contribute to future risk via kindling and relapse. The risk of home detox is not only the immediate seizure or delirium but also the higher probability of an incomplete treatment episode that ends in relapse and repeated withdrawal exposure.

How Clinicians Assess Withdrawal Severity and Risk?
CIWA-Ar: Measuring Current Symptoms
The Clinical Institute Withdrawal Assessment for Alcohol, Revised (CIWA-Ar) is one of the most widely used instruments for alcohol withdrawal symptom severity. Current summaries indicate:
- Mild: CIWA-Ar less than 10
- Moderate: CIWA-Ar 10 to 18
- Severe: CIWA-Ar 19 or higher
ASAM specifically describes severe withdrawal as CIWA-Ar 19 or higher with severe anxiety and moderate to severe tremor, and “complicated” withdrawal as severe withdrawal plus seizure, delirium-like confusion, or new hallucinations.
However, CIWA-Ar has important limitations. It depends on the patient being awake, communicative, and able to answer questions reliably. It can be confounded by coexisting illness or psychiatric symptoms. Most importantly, it measures current severity but does not by itself predict who will deteriorate later.
PAWSS: Predicting Future Complications
The Prediction of Alcohol Withdrawal Severity Scale was designed to estimate the risk of developing complicated withdrawal before symptoms fully escalate. A cutoff of PAWSS 4 or higher has been associated with high predictive value for identifying patients at risk of complicated withdrawal.
This distinction is critical for home detox decisions. A low CIWA-Ar in a patient with prior DTs and liver disease does not make home detox safe. Risk prediction matters beyond current symptoms.
Who Should Not Attempt Home Detox?
The strongest evidence-supported contraindications or red flags include:
- Prior withdrawal seizures
- Prior delirium tremens
- Multiple prior detoxifications or kindling history
- Moderate symptoms with additional risk factors
- Severe or complicated withdrawal symptoms
- Hallucinations, confusion, or clouded sensorium
- Unstable vital signs
- Serious medical illness such as liver disease, cardiac disease, infection, or head injury
- Serious psychiatric illness or suicide risk
- Pregnancy
- Age over 65
- Benzodiazepine dependence
- Inability to take oral medications
- Lack of reliable support network
- Suspected head injury
- Prior failure of ambulatory withdrawal
What Structured Ambulatory Management Looks Like?
ASAM recommends in ambulatory settings:
- Daily check-ins for up to five days after cessation or reduction of alcohol use
- Reassessment of physical condition, vital signs, hydration, orientation, sleep, and emotional status
- Validated withdrawal severity monitoring
- Additional monitoring in current or past benzodiazepine use disorder
- Education on severe symptom warning signs
- Low-stimulation home environment
- Non-caffeinated fluids
- Oral thiamine 100 mg per day for 3 to 5 days
- Medication adherence counseling
- Rapid transfer if symptoms worsen, severe tremor persists, hallucinations or confusion or seizure occurs, patient becomes oversedated, or vital signs are unstable
NICE similarly recommends fixed-dose medication regimens in community detox, tapering over 7 to 10 days, monitoring every other day, carer or family oversight of medication when possible, psychosocial support including motivational interviewing, and dose adjustment if severe symptoms or oversedation occur.
This is not “light touch” care. It is a medical program with symptom tracking, risk surveillance, and contingency planning.
Warning Signs That Home Detox is Becoming Unsafe
Guideline-supported transfer or emergency warning signs include:
- Seizure
- Hallucinations
- Confusion or clouded sensorium
- Marked agitation
- Severe tremor not resolving
- Persistent vomiting
- Unstable blood pressure or heart rate
- Syncope
- Oversedation
- Worsening medical or psychiatric condition
- Inability to maintain hydration or oral intake
If any of these occur, immediate medical evaluation is necessary.
Why Alcohol Withdrawal is Dangerous?
Alcohol withdrawal is dangerous because it is a potentially life-threatening hyperexcitable rebound state of the brain and autonomic nervous system that can progress from seemingly manageable symptoms to seizures, delirium tremens, severe autonomic instability, metabolic complications, injury, and death.
The danger is magnified by the timing of withdrawal. Symptoms may begin within hours, seizures often occur within 6 to 48 hours, and delirium tremens may emerge later, often after the patient or family falsely believes the worst has passed.
Severe withdrawal can produce tachycardia, hypertension, diaphoresis, fever, agitation, and severe tremor. Although these can be viewed as symptoms, they also signal a physiologic stress state. Unstable vital signs or syncope are indications for transfer from ambulatory management to a higher level of care.
The Role of Benzodiazepines and Medical Treatment
Benzodiazepines are the first-line treatment because they reduce withdrawal symptoms and the incidence of seizures and delirium. This is supported by ASAM and multiple evidence reviews.
Severe cases may need ICU-level care. Patients with recurrent seizures, severe altered mental status, benzodiazepine-resistant withdrawal, hyperthermia, or other ICU-level medical needs may need intensive care, second-line agents, or airway support.
Hospital care may also be necessary for continuous monitoring, IV or IM thiamine, correction of electrolytes, IV fluids, management of liver disease or infection, trauma evaluation, and delirium workup.
Common Misconceptions About Home Detox
“If I’ve done it before, I can do it again”
Repeated prior detoxifications may increase risk via kindling, not prove safety.
“I’m still awake and talking, so it can’t get serious”
Seizures and DTs often happen later, not at the first moment of quitting.
“My CIWA score is low, so I’m safe”
CIWA-Ar measures current severity, not future risk.
“I’ll just use some benzos if needed”
Unsupervised sedative use can cause oversedation, misuse, and masking of worsening withdrawal. Guidelines recommend structured regimens and supervision.
“Detox is the treatment”
Withdrawal management alone does not treat alcohol use disorder and may set up relapse and repeated future withdrawals if not linked to ongoing care.
Concrete Clinical Scenarios
Scenario 1: “I only get shaky, but I’ve had seizures before”
A person drinks heavily every day, stopped 10 hours ago, is anxious and tremulous, and says prior attempts included one seizure years ago. Current symptoms are moderate but not dramatic.
Evidence-based interpretation: High risk. Prior withdrawal seizures strongly predict future complicated withdrawal; repeated withdrawals suggest kindling. This patient should not attempt unsupervised home detox.
Scenario 2: “My symptoms are mild, but I’m alone and have cirrhosis”
A person with chronic liver disease plans to stop at home and says they can call someone if needed.
Evidence-based interpretation: Unsafe for self-detox. Liver disease is a significant complicating factor; home monitoring is inadequate, and medication choices and dosing may need adjustment.
Scenario 3: “I’m 35, healthy, no seizure history, mild symptoms, partner at home”
This patient has mild withdrawal, no serious comorbidity, no history of DTs or seizures, can attend daily monitoring, and has a supportive partner.
Evidence-based interpretation: This patient may be an appropriate ambulatory candidate, but only in a structured outpatient program, not casual self-detox.
Scenario 4: “I’m hallucinating but I know it’s withdrawal”
New auditory or visual hallucinations occur at home during detox.
Evidence-based interpretation: This is complicated withdrawal and requires urgent medical evaluation. Hallucinations are one of ASAM’s defining features of complicated withdrawal.
The Importance of Long-Term Treatment
ASAM emphasizes that withdrawal management is not effective treatment for alcohol use disorder by itself; it should be one component of engagement in ongoing treatment.
This is relevant to danger because repeated withdrawal episodes increase future withdrawal severity. A person who repeatedly detoxes at home without entering ongoing treatment may be cycling through a biologically worsening pattern. In practical terms, successful home detox that is followed by relapse and repeated future withdrawals may increase long-term risk.
Conclusion: When Home Detox Is and Isn’t Safe?
Unsupervised home alcohol detox is often more dangerous than the public assumes, and it is inappropriate for anyone with more than mild symptoms, significant risk factors, prior complicated withdrawal, major comorbidity, or unreliable support.
The biggest risks of detoxing from alcohol at home are delayed progression to seizures or delirium after initially mild symptoms, under-recognition of high-risk history, lack of structured monitoring and reliable caregiver support, unmanaged medical comorbidity, inadequate hydration and thiamine replacement, unsafe self-medication, and failure to connect withdrawal care to long-term alcohol use disorder treatment.
A medically supervised ambulatory detox program can be appropriate for carefully selected, low-risk patients with mild withdrawal, reliable support, and close follow-up. But for patients with moderate symptoms plus risk factors, any history of complicated withdrawal, major comorbidity, unstable psychiatric status, or poor social support, home detox carries risks that are not merely uncomfortable but potentially catastrophic.
The best evidence-backed position is clear: alcohol detox at home should be treated as a structured medical decision, not a casual personal experiment. If you or someone you care about is considering stopping alcohol, the safest first step is a professional assessment to determine the appropriate level of care.
If you’re ready to take that step, reach out to our team at Thoroughbred Wellness and Recovery to discuss your options and create a safe, personalized plan for recovery.









