
Methadone and weight gain go hand in hand for many people in treatment for opioid use disorder.
Research shows that patients commonly gain an average of about 18 pounds within the first two years of starting methadone, and some studies find that the share of patients classified as overweight or obese can nearly double over three years of treatment.
This article walks through what the evidence actually says, why weight changes happen, and what our professionals can do about it.
Does Methadone Cause Weight Gain? What the Evidence Shows
The short answer is yes, for most people. Multiple longitudinal studies and evidence reviews consistently find that body weight and body mass index (BMI) rise after methadone is started, often meaningfully so.
One frequently cited outpatient chart review followed 96 patients for about 1.8 years and found that mean BMI rose from 27.2 to 30.1, which worked out to an average gain of roughly 18 pounds.
About 65 percent of patients in that study gained at least 5 percent of their body weight, a threshold the researchers considered clinically significant. Women gained considerably more than men, averaging about 28 pounds compared to about 12 pounds for men.
A separate three-year study of 74 patients found an even starker picture. The proportion classified as overweight, obese, or morbidly obese rose from 42 percent at admission to 76 percent at year one, 82 percent at year two, and 88 percent by year three. Blood pressure, blood sugar, and cholesterol levels also tended to worsen over that same period.
A recent scoping review that examined 21 studies concluded that methadone treatment appears associated with mild to moderate weight gain, with six-month gains ranging from about 4 to 23 pounds across studies. Nine of eleven studies that reported BMI found significant increases.
So the evidence is not subtle. Weight gain during methadone maintenance is common, often substantial, and clinically meaningful.
How Much Weight, and How Fast?
The timing matters as much as the total amount. The pattern that emerges across studies looks roughly like this:
- Noticeable gain often begins within the first few months of treatment.
- The first year tends to show the largest increases.
- Some patients continue gaining into years two and three.
- Other patients stabilize after the first year or two.
A four-year observational study found that average weight rose from about 65 kg at entry to about 73 kg at one year and 75 kg at two years, with no statistically significant increase after that point. That suggests the first year or two may be the most critical window for intervention.
Is the Weight Gain Just Fat, or Something Else?
This is an important question. Some weight gain during early recovery reflects a return to healthier nutrition after a period of active opioid use, when eating is often irregular and the body is under significant stress. That kind of gain is not necessarily harmful.
But body composition data tell a more concerning story. One study found that within a year of starting methadone, body fat percentage increased from about 25 percent to about 31 percent, while muscle mass fell from about 71 percent to about 66 percent.
That pattern, more fat and less muscle, is not simply healthy recovery weight. It points toward a real shift in metabolic health, not just a return to a normal baseline.
Why Does Methadone Make You Gain Weight?
The honest answer is that several things are happening at once, and no single explanation covers every patient. The research supports a layered model.
Recovery from Undernutrition
Before treatment, many people with active opioid use disorder eat irregularly, live under chaotic conditions, and often lose weight because of illness, poverty, and the physical demands of addiction.
When methadone stabilizes opioid use, appetite returns, meals become more regular, and sleep improves. Some weight gain is simply the body catching up.
A review of weight management strategies in methadone maintenance treatment notes that individuals in early recovery may eat a high-calorie diet partly to compensate for a reward system that has been suppressed by prolonged opioid use. That is a behavioral and neurobiological explanation, not a moral one.
Increased Craving for Sweet Foods
One of the most consistently reported findings in this literature is that people on methadone tend to prefer sweet and highly palatable foods.
A study examining eating behavior and nutrition knowledge among methadone patients found that worse diet habits and desire for sweet foods were directly linked to higher BMI.
This is biologically plausible because opioid receptors are involved in the brain’s reward circuitry, which governs both drug use and food intake. When opioid use decreases, some people shift toward food, especially sweets, as a source of reward.
Metabolic Changes
Methadone may also affect how the body handles glucose and fat. A comparison of patients on methadone versus buprenorphine found that methadone was associated with worse metabolic profiles, including higher rates of insulin resistance, worse triglyceride and HDL cholesterol levels, and higher fasting glucose.
A 2023 narrative review of metabolic changes in opioid use disorder similarly concluded that methadone treatment appears linked to weight gain, dyslipidemia, and hyperglycemia in some patients.
Social and Environmental Factors
Patients in methadone programs often face poverty, food insecurity, limited access to healthy food, sedentary routines, and co-occurring psychiatric conditions.
Many also take other medications, including antidepressants or antipsychotics, that can independently promote weight gain. These factors do not make methadone less responsible, but they do mean that the medication is rarely the only driver.
Who is More Likely to Gain Weight on Methadone?
The research is not perfectly consistent, but a few patterns appear across studies.
The following factors have been associated with greater weight gain in at least some studies:
- Female sex (though a meta-analysis of four studies found the difference was not statistically significant overall)
- Black or African American race (noted in one three-year study, though racial disparities remain underexamined across the broader literature)
- Higher methadone doses (found in some studies but not others, so this is not a settled predictor)
- Better baseline health, such as being hepatitis C negative or not using benzodiazepines, which may reflect greater capacity to gain weight once stabilized
One finding that surprises people is that healthier patients at admission sometimes gain more weight.
A plausible explanation is that they are better positioned to remain in treatment, eat more consistently, and respond more fully to the stabilizing effects of the medication.
Methadone Weight Loss: When Does It Happen?
While weight gain is the dominant pattern, some people do lose weight while taking methadone. This is less common and usually points to something specific going wrong rather than a direct effect of the medication itself.
FDA labeling for methadone explicitly lists weight loss as part of the opioid withdrawal symptom cluster, alongside nausea, vomiting, diarrhea, anorexia, and abdominal cramps.
This matters because it tells us that weight loss on methadone is most likely to occur when the dose is too low, when the patient is not yet stabilized, or when doses are missed or the medication is tapered too quickly.
Other reasons someone might lose weight while taking methadone include:
- Nausea or vomiting as a side effect, especially early in treatment
- Continued use of stimulants like cocaine or methamphetamine, which suppress appetite
- Co-occurring illness such as infection or depression
- Food insecurity or housing instability
- Drug interactions that affect appetite or metabolism
Unexplained weight loss during methadone treatment is a clinical signal worth investigating, not something to dismiss as a routine variation.
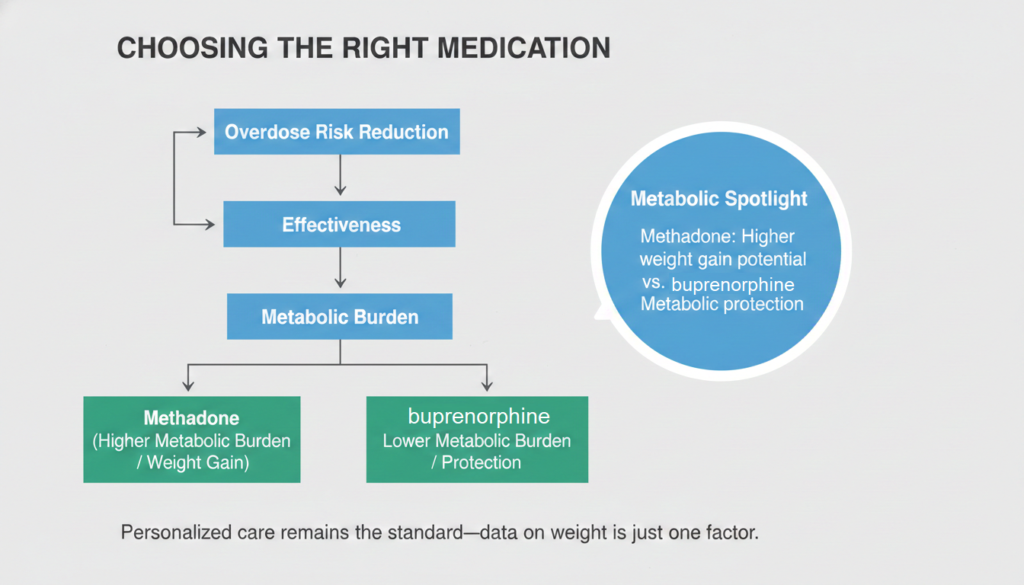
Methadone vs. Buprenorphine and Naltrexone: Does the Choice of Medication Matter?
The evidence here is limited but suggestive. Methadone appears to carry a somewhat greater metabolic burden than buprenorphine.
The comparison study mentioned earlier found that while both groups were overweight or obese and insulin resistant, buprenorphine patients had better HDL values and lower rates of metabolic syndrome overall.
For naltrexone, a small six-month comparison found no statistically significant difference in weight change between methadone and naltrexone groups, though the sample was too small to draw firm conclusions.
Some research suggests naltrexone may reduce preference for sweet foods, which could theoretically offer some metabolic protection, but this has not been well studied in opioid use disorder populations specifically.
None of this means buprenorphine or naltrexone are automatically better choices for every patient. Methadone remains one of the most effective treatments for opioid use disorder, and the decision about which medication to use should be based on the full clinical picture, not weight concerns alone.
Why This Matters: The Real Health Stakes
Weight gain during methadone treatment is not just a cosmetic concern. The three-year study that tracked BMI also tracked cardiovascular risk factors, and the findings were clear: as BMI rose, rates of hypertension, diabetes, and high cholesterol rose alongside it. Increasing BMI in methadone patients has also been linked to sleep breathing disorders, including obstructive sleep apnea.
A 2023 narrative review confirmed that opioid use before recovery is often associated with lower body weight, meaning the shift into treatment can trigger a significant metabolic transition.
When that transition leads to excess fat gain rather than healthy weight restoration, the long-term consequences can include cardiovascular disease, type 2 diabetes, and reduced quality of life.
This does not mean methadone should be avoided. Its benefits for reducing overdose deaths, illicit drug use, and infectious disease transmission are too well established to dismiss.
But it does mean that weight and metabolic health should be treated as part of routine care from the very start of treatment, not addressed only after problems develop.
What Can Be Done About Methadone-Related Weight Gain?
The research on interventions is still limited, but a few things are clear.
A randomized trial of a brief nutrition education program for methadone patients found that knowledge and self-reported food habits improved in the intervention group, though BMI did not change over the six-week follow-up period.
That result is not surprising. Six weeks is not long enough to change body weight, and knowledge alone rarely changes behavior without ongoing support.
What the evidence does support is starting early. Because weight gain often begins within the first months of treatment, waiting until a patient is already obese to address nutrition and lifestyle is too late.
Clinicians should discuss the likelihood of weight change at treatment initiation, monitor weight and metabolic markers regularly, and connect patients with nutrition support as part of standard care.
Monitoring should include:
- Body weight and BMI at regular intervals
- Blood pressure
- Fasting glucose or hemoglobin A1C
- Lipid panel
- Assessment of diet quality and sweet food cravings
- Review of all co-prescribed medications that may affect weight
The American Diabetes Association’s 2026 standards on obesity care emphasize person-centered, shared decision-making approaches to weight management, including regular nutrition counseling and monitoring.
That framework applies directly to methadone patients, who deserve the same quality of chronic disease management as anyone else.
The Bottom Line on Methadone and Weight Changes
Methadone does not make every patient gain weight, and it does not cause weight loss in most patients on stable maintenance doses.
What it does is create a treatment context in which weight gain is common, often clinically meaningful, and driven by a mix of pharmacologic, behavioral, metabolic, and social factors.
The most accurate way to think about it is this: methadone is associated with weight gain in many patients, and that association is strong enough to treat as a real and expected part of treatment rather than a rare side effect.
At the same time, some patients lose weight, usually because of withdrawal symptoms, inadequate dosing, side effects, or co-occurring conditions rather than because methadone itself promotes weight loss.
The right response is not to avoid methadone when it is the best option for treating opioid use disorder. The right response is to treat weight and metabolic health as part of whole-person care from day one.
If you or someone you care about is navigating opioid use disorder and has questions about treatment options, medication effects, or what recovery can look like, speaking with our qualified clinical team makes a real difference.
Thoroughbred Wellness and Recovery offers Methadone addiction treatment with integrated medical and behavioral support to help you move forward with clarity and confidence.









