
If you suspect kratom has shifted from a choice to a need, you are not alone and you are not imagining it.
Research shows that about one third of regular U.S. kratom users in one online convenience sample met criteria for kratom use disorder.
This guide will help you spot the signs of kratom addiction, understand what withdrawal feels like, and learn which treatment paths have the strongest evidence behind them.
Recognizing Kratom Addiction Signs
Kratom does not have its own standalone diagnosis in the DSM-5, which makes it easy to dismiss growing dependence as “just a supplement habit.” But the pharmacology tells a different story.
The plant’s main alkaloids, mitragynine and 7-hydroxymitragynine, act on mu-opioid receptors. That same receptor activity that can ease pain or calm withdrawal is also what creates tolerance, physical dependence, and craving over time.
A 2023 scientific expert forum concluded that kratom dependence is real, underrecognized, and most visible in people who dose multiple times daily, use concentrated extracts, or rely on kratom as an opioid substitute.
The risk is not all or nothing. It sits on a spectrum shaped by dose, frequency, duration, product potency, and personal vulnerability.
Behavioral and Physical Warning Signs
The clearest signs of kratom addiction mirror patterns seen across substance use disorders, but they carry a few kratom-specific twists.
- Needing higher doses or stronger products (such as extract shots) to feel the same effect
- Dosing mainly to avoid feeling sick, achy, or anxious rather than to gain any positive benefit
- Repeated failed attempts to cut back or quit
- Structuring the day around dosing times and feeling panicked when supply runs low
- Hiding use from partners, family, or doctors, often rationalizing it as “just a supplement”
- Continuing use despite worsening sleep, mood, liver function, weight loss, or relationships
- Switching from traditional leaf powder to concentrated 7-hydroxymitragynine products because plain kratom “stopped working”
- Using kratom to self-treat opioid withdrawal, then becoming dependent on kratom itself
That last point shows up repeatedly in case literature. One early report documented a patient who began kratom for opioid withdrawal and chronic pain, only to develop a new dependence pattern on kratom.
Later cases describe the same cycle with escalating severity, including psychiatric destabilization and emergency hospitalization.
When “Use” Becomes “Addicted to Kratom”?
Not every person who tries kratom becomes addicted. A practical way to think about it is a four-stage continuum.
| Stage | Typical Features | Addiction Likelihood |
|---|---|---|
| Occasional use | Infrequent, no withdrawal, no impairment | Low |
| Regular use | Repeated dosing for pain, mood, or energy; still feels controlled | Variable |
| Physical dependence | Withdrawal on stopping, tolerance, frequent dosing | Moderate to high |
| Addiction / kratom use disorder | Compulsive use, failed quit attempts, cravings, continued use despite harm | High |
You are likely addicted to kratom if you cannot comfortably stop, your use has escalated, you get withdrawal symptoms, you have lost control over the pattern, and you keep using despite clear harm. That cluster, not any single symptom, is the most reliable indicator.
How Kratom Withdrawal Feels?
Withdrawal is often the moment a person realizes kratom has become a problem. The symptom profile resembles opioid withdrawal, though a scientific expert forum found it is often milder on average and more variable from person to person.
Physical Symptoms
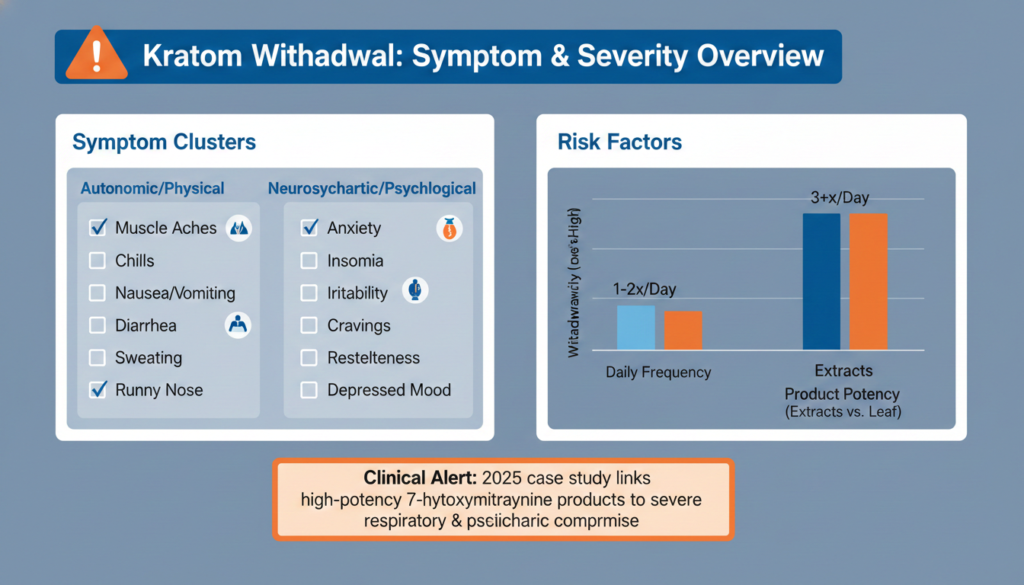
Commonly reported physical symptoms include muscle aches, joint pain, sweating, chills, nausea, diarrhea, abdominal cramps, runny nose, watery eyes, tremors, loss of appetite, and feverish sensations. These tend to peak within the first few days after stopping.
Psychological Symptoms
Anxiety, irritability, restlessness, depressed mood, insomnia, difficulty concentrating, and intense cravings are frequently described across field studies and clinical reviews.
For people who started kratom to manage anxiety or depression, withdrawal can feel like a return of the original condition layered on top of new discomfort.
Severity Depends on the Details
Withdrawal intensity is not uniform. Frequency of use may predict dependence more reliably than dose size alone. Someone dosing multiple times every day for months, especially with concentrated extracts, faces a harder withdrawal than someone who used plain leaf tea a few times a week.
A 2025 case involving concentrated 7-hydroxymitragynine products resulted in severe withdrawal with psychosis and respiratory compromise that needed intensive care. That outcome is rare, but it shows that newer high-potency products can shift the risk profile well beyond what older assumptions about kratom would suggest.
Kratom Withdrawal Treatment Options
There are no FDA-approved medications specifically for kratom withdrawal, and no randomized controlled trials have been completed.
That does not mean clinicians are guessing. The case literature and expert commentary are now consistent enough to support a stepped-care approach matched to severity.
Tapering and Symptomatic Care
For mild to moderate withdrawal, gradual tapering is one of the most consistently endorsed strategies. The 2023 expert forum specifically recommended evaluating gradual kratom dose reduction alongside non-opioid agents like clonidine and lofexidine for autonomic symptoms.
Practical symptom management often includes anti-nausea medication, sleep aids, analgesics for body aches, and hydration monitoring.
Tapering works best when the person uses a consistent product, can measure and reduce intake, and has a stable environment.
It works poorly when the product potency varies batch to batch, cravings are overwhelming, or an untreated pain or psychiatric condition keeps pulling the person back.
Buprenorphine for Severe Cases
Buprenorphine-naloxone is the most promising medication option for people with severe kratom withdrawal, repeated failed quit attempts, or overlapping opioid use disorder.
A 28-patient case series found that most patients stabilized on 8 to 16 mg of buprenorphine-naloxone, with 82% testing negative for mitragynine at both 8 and 12 weeks. Twenty of the 28 patients stayed in treatment for 5 to 22 months.
Earlier case reports showed similar results. Two patients with chronic pain who had turned to kratom after losing opioid prescriptions were successfully transitioned to buprenorphine-naloxone, which controlled both withdrawal and pain.
Buprenorphine is especially appropriate when kratom use is really an extension of opioid use disorder. In those situations, treating only the kratom layer while ignoring the underlying opioid dependence sets the person up for relapse to illicit opioids.
Other Medication Options
Methadone appears in a small number of inpatient cases, typically paired with clonidine for symptom-driven dosing. Naltrexone has been used after successful detox in selected patients.
Clonidine and lofexidine remain the best-supported non-opioid adjuncts for autonomic symptoms like sweating, agitation, and elevated heart rate. None of these options has as much practical support in the current literature as buprenorphine for persistent, severe kratom use disorder.
Behavioral and Psychosocial Support
Quitting kratom without addressing the reason you started is a recipe for relapse. Cognitive behavioral therapy, motivational interviewing, peer support groups, and relapse-prevention planning all play a role.
A recent review noted that psychotherapy and contingency management are unlikely to cause harm and may be reasonable for any severity level of kratom use disorder.
This matters because kratom often fills a gap. If that gap is chronic pain, untreated anxiety, depression, or trauma, the gap will still be there after detox unless someone treats it directly.
Matching Treatment to Your Situation
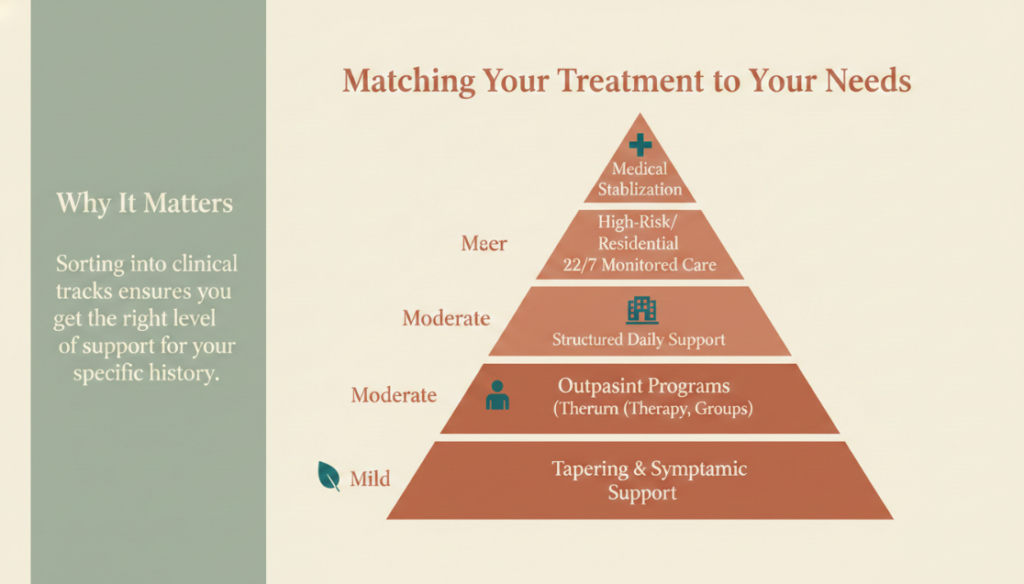
The strongest recent evidence supports sorting people into clinical tracks rather than applying one protocol to everyone.
Mild isolated withdrawal, first quit attempt. Outpatient tapering, symptomatic medications, and behavioral follow-up are usually enough.
Moderate withdrawal without opioid use disorder history. Structured outpatient or intensive outpatient care with clonidine or lofexidine, therapy, and frequent check-ins.
Severe withdrawal, repeated relapses, or high-dose long-term use. Buprenorphine-naloxone should be actively considered, not reserved as a last resort.
Kratom used to self-treat opioid withdrawal or known opioid use disorder. Treat the opioid use disorder directly. Buprenorphine is often the most evidence-consistent choice.
Significant medical or psychiatric instability, polysubstance use, or unsafe home environment. A higher level of care such as residential or inpatient withdrawal management is safer.
Why Detox Alone is Not Enough?
ASAM’s broader treatment principles make a point that applies directly to kratom: withdrawal management by itself is not effective treatment. It should be the start of ongoing care, not the finish line.
SAMHSA defines recovery as a process of change through which people improve health, live self-directed lives, and work toward their full potential.
For someone quitting kratom, durable success depends on treating the underlying drivers of use, whether that is chronic pain, anxiety, depression, PTSD, or opioid dependence. It also depends on stable housing, social support, relapse-prevention skills, and continued follow-up.
Detox clears the substance from your body. Everything after detox determines whether it stays cleared.
Moving Forward With Confidence
Kratom addiction is real, it is underrecognized, and it responds to structured treatment. If you see yourself in the signs described here, that awareness is already a step forward.
The evidence says you do not have to white-knuckle through withdrawal alone, and you do not have to figure out the right level of care by yourself.
If you or someone you care about is struggling with kratom or any substance, reaching out for professional guidance can make the difference between another failed attempt and lasting change.
Contact Thoroughbred Wellness & Recovery to talk through your options with a team that treats addiction and mental health together.









